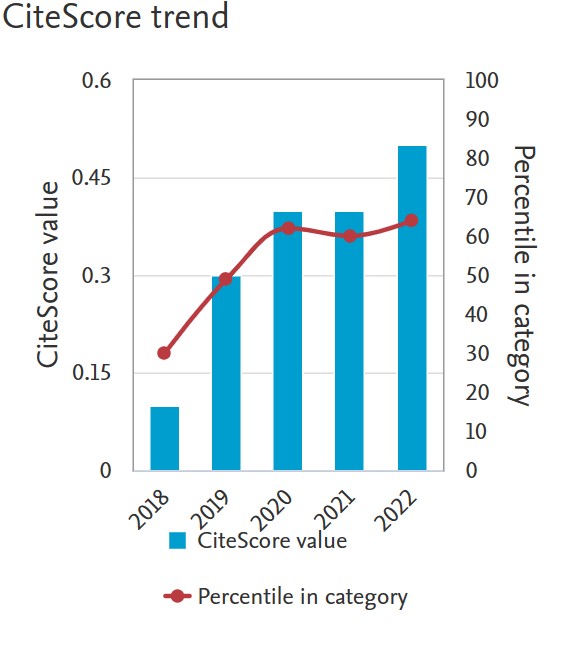
Pregnancy and left ventricular Echocardiography parameter
Keywords:
left ventricular function, pregnancy, and echocardiography.Abstract
Background: Profound maternal hemodynamic changes occur in order to satisfy the demands of a growing foetus. Early in pregnancy, peripheral vascular resistance (PVR) lowers, generating a considerable rise in cardiac output. Many parameters are employed for measuring the LV systolic function with different echocardiographic modalities including: M-Mode echocardiography, two-dimensional echocardiography, three-dimensional echocardiography, tissue doppler imaging. Objective: To determine the effects of first pregnancy on the LV systolic and diastolic function using Echocardiography. Subjects and Methods: This is a cross sectional study, conducted at Baghdad medical city in the time period from August 2020 to January 2021. Patients and controls were recruited among individuals attending the Obstetrics and Gynecology department and examined in the department of echocardiography and catheterization of the same hospital. A total of 80 women were enrolled in this study, and they were categorized into two groups: A set of 40 non pregnant women with mean age (24 ±3 year) served as controls. 40 pregnant women with normal singleton pregnancy (30-40 weeks of gestation) with mean age (23±2.6 year) served as study group. Results: the studied groups showed no significant difference in height and age with a significant increase in body weight in the study group over the control. Pregnant female group had mean BMI and BSA significantly higher than control group. Pregnant female group had a significant increase in Left ventricular internal dimensions during diastole (LVIDd) over controls, the Interventricular septal thickness (IVS) was significantly higher in pregnant female than controls. In pregnant women the A wave velocity didn’t have a significant difference compared to the control group, while E wave velocity and E/A ratio was significantly lower in pregnant women than controls, LA area was significantly higher in pregnant women over controls. Conclusions: Echocardiography isvery useful to determine the effects of first pregnancy on the LV systolic and diastolic function.
Downloads
References
Meah VL, Cockcroft JR, Backx K, Shave R,
Stohr EJ. (2016). Cardiac output and related
haemodynamics during pregnancy: a series of
meta-analyses. Heart; 102:518—526.
Silversides, CKand Coleman, JM. (2011). In:
Oakley C, Warnes CA, editors, (eds.).
Physiologic changes in pregnancy. Heart
Disease in Pregnancy. (2nd ed) Malden, MA:
Blackwell Publishing; 6-17.
Ducas RA, Elliott JE, Melnyk SF, Premecz S,
daSilva M, Cleverley K, Wtorek P, Mackenzie
GS, Helewa ME, Jassal DS.
(2014).Cardiovascular magnetic resonance in
pregnancy: insights from the Cardiac
Hemodynamic Imaging and Remodeling in
Pregnancy (CHIRP) study. J Cardiovasc
Magn Reson; 16:1.
Barrett,KE.,Boitano, S., Barman, SM. and
Brooks, HL. (2012). Ganong's Review of
Medical Physiology. (24e), Philadelphia:
Saunders, pp. 103g.
Fyhrquist, F. and Saijonmaa, O. (2008).
Renin-angiotensin system revisited. J Intern
Med., (264):224—236.
Al-Alwany A. Assessment of Left Ventricular
Function in Body builders using conventional
echocardiography: ANNALS OF
TROPICAL MEDICINE AND PUBLIC
HEALTH - Volume 24 Issue 6, April - 2021
Pages: 561-569
Kanai, E., Barkovich,AJ., Bell, C.et al.(2007).
Blue Ribbon Panel on MR Safety. ACR
guidance document for safe MR practices.
AJR Am J Roentgenol, (188):1447—1474.
Kametas, NA., McAuliffe, F., Hancock, J.et
al. (2001). Maternal left ventricular mass and
diastolic function during pregnancy.
Ultrasound Obstet Gynecol., (18): 460—466.
Mesa A., Jessurun C., Hernandez A.et al.
(1999). Left Ventricular Diastolic Function in
Normal Human Pregnancy. Circulation,
(99):511- 517.
Valensise, H, Vasapollo, B, Novelli, GP,
Larciprete, G, Romanini, ME, Arduini, D,
Galante, A andRomanini, C. (2001). Maternal diastolic function in asymptomatic pregnant
women with bilateral notching of the uterine
artery waveform at 24 weeks’ gestation: a pilot
study. Ultrasound Obstet Gynecol., 18:450—
Melchiorre K., Sutherland G.R., Baltabaeva
A., Liberati M., Thilaganathan B.(2011).
Maternal Cardiac Dysfunction and
Remodeling in Women with Preeclampsia at
Term. Hypertension, (57):85-93.
Garabed Eknoyan, 2007. Obesity, diabetes,
and chronic kidney disease,
Curr Diab Rep;7(6):449-53.
Mosteller, 1987. Simplified calculation of
body-surface area, N Engl J Med
;317(17):1098.
Lang, R.M., Badano, L.P., Mor-Avi, V.,
Afilalo,J., Armstrong A. (2015).
Recommendations for Cardiac Chamber
Quantification by Echocardiography in
Adults: An Update from the American Society
of Echocardiography and the European
Association of Cardiovascular Imaging.
Journal of the American Society of
Echocardiography, (8): 1-5.
Solomon SD, Wu JC and Gillam L (2019):
Echocardiography. In: Mann DL, Zipes DP,
Libby P, Bonow RO. Braunwald's Heart
Disease: A Textbook of Cardiovascular
Medicine. 11th ed. Elsevier Saunders:
Philadelphia; 179-192.
Troiano, N. H. (2018). Physiologic and
hemodynamic changes during pregnancy.
AACN advanced critical care, 29(3), 273-283.
Umesawa, M., & Kobashi, G. (2017).
Epidemiology of hypertensive disorders in
pregnancy: prevalence, risk factors, predictors
and prognosis. Hypertension Research, 40(3),
-220.
Villamor, E., Tedroff, K., Peterson, M.,
Johansson, S., Neovius, M., Petersson, G., &
Cnattingius, S. (2017). Association between
maternal body mass index in early pregnancy
and incidence of cerebral palsy. Jama, 317(9),
-936.
Kutchi, L, Chellammal, P., & Akila, A.
(2020). Maternal obesity and pregnancy
outcome: in perspective of new Asian Indian
guidelines. The Journal of Obstetrics and
Gynecology of India, 1-7.
Kolovetsiou-Kreiner, V., Moertl, M. G.,
Papousek, L, Schmid-Zalaudek, K., Lang,
U., Schlembach, D., ... & Lackner, H. K.
(2018). Maternal cardiovascular and
endothelial function from first trimester to
postpartum. PloS one, 13(5), e0197748.
Garg, P., Yadav, K., Jaryal, A. K., Kachhawa,
G., Kriplani, A., & Deepak, K. K. (2020).
Sequential analysis of heart rate variability,
blood pressure variability and baroreflex
sensitivity in healthy pregnancy. Clinical
Autonomic Research, 30(5), 433-439.
Ngene, N. C„ & Moodley, J. (2019).
Physiology of blood pressure relevant to
managing hypertension in pregnancy. The
Journal of Maternal-Fetal & Neonatal
Medicine, 32(8), 1368-1377.
Charkoudian, N., Usselman, C. W., Skow, R.
J., Staab, J. S., Julian, C. G., Stickland, M.
K., ... & Steinback, C. D. (2017). Muscle
sympathetic nerve activity and volume¬
regulating factors in healthy pregnant and
nonpregnant women. American Journal of
Physiology-Heart and Circulatory
Physiology, 313(4), H782-H787.
Tomo, A., Rupinder, K., Anthony, A. H.,
Allison, B., Kana, F., Cynthia, C.T. (2015).
Physiological adaptation of the left ventricle
during the second and third trimesters of a
healthy pregnancy: a speckle tracking
echocardiography study. Am J Cardiovasc
Dis.,5(2):119-126.
Kawamatsu, N., Ishizu, T., & Kawakami, Y.
(2019). What we know and what we don’t
know about the adaptation to pregnancy and
left ventricular diastolic dysfunction. Circulation Journal, CJ-19.
Moran AM, Colan SD, Mauer MB, Geva T.
(2002). Adaptive mechanisms of left
ventricular diastolic function to the
physiologic load of pregnancy. Clin Cardiol;
:124.
Tasar O, Kocabay G, Karagoz A, Kalayci
Karabay A, KarabayCY, Kalkan S, et al.
(2019). Evaluation of left atrial functions by 2-
dimensional speckle-tracking
echocardiography during healthy pregnancy. J
Ultrasound Med; 38:2981-8.
Selma, A. R. I., Hasan, A. R. ., Yilmaz, M.,
& Bozat, T. (2020) Evaluation of myocardial
function in pregnant women with speckle¬
tracking echocardiography. The European
Research Journal, 6(6), 615-623.
Al-Alwany A. Dual and Multiple AV Nodal
Pathways, What is The Deference in Typical
Atrioventricular Nodal Reentrant
Tachycardia. Medical Journal of Babylon Vol.
- No. 2 : 382 - 388 , 2017
http://www.medicaljb.com ISSN 2312-
©2017
Bansal M, Sengupta PP (2013) Longitudinal
and circumferential strain in patients with
regional LV dysfunction. Curr Cardiol Rep
:339
Al-Alwany A. Iatrogenic atrial septal defect
post radiofrequency ablation in patients with
left atrial SVT: predictors and outcome.
Revista Latinoamericana de Hipertension.
Vol. 16-ND3, 2021
Downloads
Published
Issue
Section
License
You are free to:
- Share — copy and redistribute the material in any medium or format for any purpose, even commercially.
- Adapt — remix, transform, and build upon the material for any purpose, even commercially.
- The licensor cannot revoke these freedoms as long as you follow the license terms.
Under the following terms:
- Attribution — You must give appropriate credit , provide a link to the license, and indicate if changes were made . You may do so in any reasonable manner, but not in any way that suggests the licensor endorses you or your use.
- No additional restrictions — You may not apply legal terms or technological measures that legally restrict others from doing anything the license permits.
Notices:
You do not have to comply with the license for elements of the material in the public domain or where your use is permitted by an applicable exception or limitation .
No warranties are given. The license may not give you all of the permissions necessary for your intended use. For example, other rights such as publicity, privacy, or moral rights may limit how you use the material.