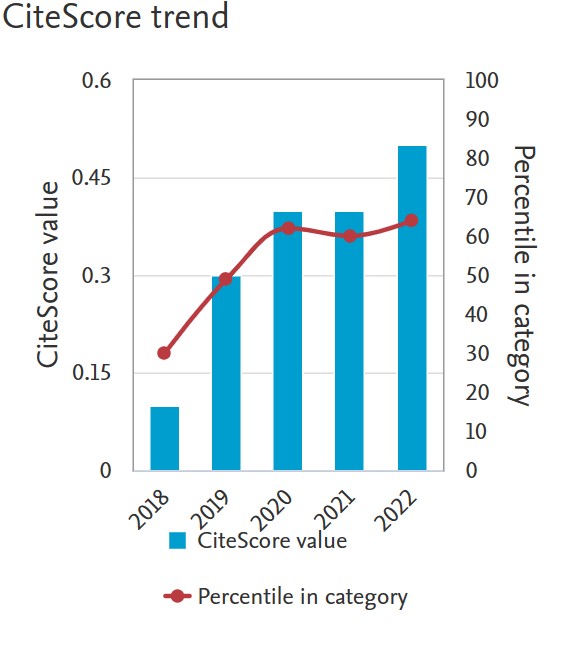
The Level of T Cells Specific to the SARS-Cov-2 Virus and Asymptomatic Infection and the Immunogenicity of a Vaccine.
Keywords:
T- cell, SARS-Cov2, 1L2, IFN, cytokineAbstract
A robust T cell response can lead to milder infections. It can also establish memory pools and can respond to certain SARS-CoV-2 variants. T cells are mainly directed toward epitopes that are part of conserved peptides. Although the effects of IL2 and IFN on long-term immunity are still unclear, it is believed that these two factors play a role in the development of TH1 responses in uninfected individuals. By analyzing the responses of the participants, we were able to determine that 9 out of the 11 individuals exhibited dual-producing IFN/IL-2+ T cells, decreasing to 8 out of 10 for the asymptomatic group. The reduction in the levels of 1L2 in THltype cells, which came from asymptomatic infection, has made it possible to predict the response of T cells to IFN in people with no previous history of infection or vaccination. After the first vaccination, the not-vaccinated participants had a high level of IL-2 response. Compared to AstraZeneca's vaccine, the Pfizer vaccine was more likely to elicit a higher L2 response. On the other hand, the IFN response of the AstraZeneca vaccine was not significantly different from that of the Pfizer vaccine.
Downloads
References
Ahmed, S. F., Quadeer, A. A., & McKay, M.
R. (2020). Preliminary identification of
potential vaccine targets for the COVID-19
Coronavirus (SARS-CoV-2) Based on SARSCoV Immunological Studies. Viruses, 12(3).
https://doi.org/10.3390/vl2030254
Ameratunga, R., Longhurst, H., Steele, R.,
Lehnert, K., Leung, E., Brooks, A. E. S., &
Woon, S. T. (2021). Common Variable
Immunodeficiency Disorders, T-Cell
Responses to SARS-CoV-2 Vaccines, and the
Risk of Chronic COVID-19. Journal of Allergy
and Clinical Immunology: In Practice, 9(10).
https://doi.Org/10.1016/j.jaip.2021.06.019
Biswas, B., Chattopadhyay, S., Hazra, S.,
Hansda, A. K., & Goswami, R. (2022). COVID-
pandemic: the delta variant, T-cell responses,
and the efficacy of developing vaccines. In
Inflammation Research (Vol. 71, Issue 4).
https://doi.oig/10.1007/s00011-022-01555-5
Bitoun, S., Henry, J., Desjardins, D„ VauloupFellous, C., Dib, N., Belkhir, R., Mouna, L„ Joly,
C., Bitu, M„ Ly, B„ Pascaud, J., Seror, R„ Roque
Afonso,A. M„ Le Grand, R., & Mariette,X. (2022).
Rituximab Impairs B Cell Response But Not T Cell
Response to COVID-19 Vaccine in Autoimmune
Diseases. Arthritis and Rheumatology, 74(6).
https://doi.oig/10.1002/art.42058
Castillo, P., Ogando-Rivas, E., Jones, N.,
Trivedi, V., Mendez-Gomez, H., Guimaraes,
F., Yang, C., Wingard, J., Sayour, E., &
Mitchell, D. (2021). Ex vivo activation of
SARS-COV-2 specific t cells using RNAloaded human antigen presenting cells.
Pediatric Blood and Cancer, 6VSUPPL 3).
Grifoni, A., Weiskopf, D., Ramirez, S. I., Mateus,
J., Dan, J. M., Moderbacher, C. R., Rawlings, S.
A., Sutherland, A., Premkumar, L., Jadi, R. S.,
Marrama, D., de Silva, A. M., Frazier, A., Carlin,
A. F., Greenbaum, J.A, Peters, B., Krammer, F.,
Smith, D. M., Crotty, S., & Sette, A. (2020).
Taigets of T Cell Responses to SARS-CoV-2
Coronavirus in Humans with COVID-19 Disease
and Unexposed Individuals. Cell, 181(7).
https://doi.Org/10.1016/j.cell.2020.05.015
He, Q., Mao, Q., An, C., Zhang, J., Gao, F.,
Bian, L., Li, C., Liang, Z., Xu, M., & Wang, J.
(2021). Heterologous prime-boost: breaking the
protective immune response bottleneck of
COVID-19 vaccine candidates. Emerging
Microbes and Infections, 10().
https://doi.oig/10.1080/22221751.2021.190224
Heitmann, J. S., Bilich, T., Tandler, C.,
Nelde, A., Maringer, Y., Marconato, M.,
Reusch, J., Jager, S., Denk, M., Richter, M.,
Anton, L., Weber, L. M., Roerden, M.,
Bauer, J., Rieth, J., Wacker, M., Horber, S.,
Peter, A., Meisner, C„ ... Walz, J. S. (2022). A
COVID-19 peptide vaccine for the induction
of SARS-CoV-2 T cell immunity. Nature,
(7894). https://d0i.0rg/l 0.1038/s41586-
-04232-5
Ishii, H., Nomura, T., Yamamoto, H.,
Nishizawa, M.,Thu Hau, T.T., Harada, S., Seki,
S., Nakamura-Hoshi, M., Okazaki, M., Daigen,
S., Kawana-Tachikawa, A., Nagata, N., IwataYoshikawa, N., Shiwa, N., Suzuki, T., Park, E.
S., Ken, M., Onodera, T., Takahashi, Y, ...
Matano, T. (2022). Neutralizing-antibodyindependent SARS-CoV-2 control correlated
with intranasal-vaccine-induced CD8+ T cell
responses. Cell Reports Medicine, 3(2).
https://doi.oig/10.1016/j.xcrm.2022.100520
Jung, M. K., & Shin, E. C. (2021). Phenotypes
and functions of sars-cov-2-reactive t cells. In
Molecules and Cells (Vol. 44, Issue 6).
https://doi.oig/10.14348/molcells.2021.0079
Kalimuddin, S., Tham, C. Y. L,, Qui, M., de
Alwis, R., Sim, J. X. Y., Lim, J. M. E., Tan,
H. C., Syenina, A., Zhang, S. L., Le Bert, N.,
Tan, A. T., Leong, Y. S., Yee, J. X., Ong, E.
Z., Ooi, E. E., Bertoletti, A., & Low, J. G.
(2021). Early T cell and binding antibody
responses are associated with COVID-19
RNA vaccine efficacy onset. Med, 2(6).https://doi.Org/10.1016/j.medj.2021.04.003
Lozano-Ojalvo, D., Camara, C., LopezGranados, E., Nozal, P., del Pino-Molina, L.,
Bravo-Gallego, L. Y, Paz-Artal, E., Pion, M.,
Correa-Rocha, R., Ortiz, A., Lopez-Hoyos, M.,
Iribarren, M. E., Portoles, J., Rojo-Portoles, M.
P., Ojeda, G., Cervera, L, Gonzalez-Perez, M.,
Bodega-Mayor, L, Montes-Casado, M., ...
Ochando, J. (2021). Differential effects of the
second SARS-CoV-2 mRNA vaccine dose on T
cell immunity in naive and COVID-19 recovered
individuals. Cell Reports, 36(8).
https://doi.oig/10.1016/j.celrep.202L109570
Madelon, N„ Heikkila, N., Royo, I. S.,
Fontarmaz, P., Breville, G., Lauper, K.,
Goldstein, R., Grifoni, A., Sette, A., Siegrist,
C. A., Finckh, A., Lalive, P. H.,
Didierlaurent, A. M., & Eberhardt, C. S.
(2022). Omicron-Specific Cytotoxic T-Cell
Responses After a Third Dose of mRNA
COVID-19 Vaccine Among Patients With
Multiple Sclerosis Treated With Ocrelizumab.
JAMA Neurology,
(4).hitps://doi.org/10.1001/jamaneurol.20
0245
Mateus, J., Dan, J. M., Zhang, Z.,
Moderbacher, C. R., Lammers, M.,
Goodwin, B., Sette, A., Crotty, S., &
Weiskopf, D. (2021). Low-dose mRNA-1273
COVID-19 vaccine generates durable
memory enhanced by cross-reactive T cells.
Science, 374(6566).
https://doi.org/10.1126/science.abj9853
Niessl, J., Sekine, T., & Buggert, M. (2021). T
cell immunity to SARS-CoV-2. In Seminars in
Immunology (Vol. 55).
https://doi.Org/10.1016/j.smim.2021.101505
Rice, A., Verma, M., Shin, A, Zakin, L., Sieling,
P., Tanaka, S., Balint, J., Dinkins, K., Adisetiyo,
H., Morimoto, B., Higashide, W., Anders Olson,
C., Mody, S., Spilman, P., Gabitzsch, E., Safrit,
J. T., Rabizadeh, S., Niazi, K., & Soon-Shiong,
P. (2021). Intranasal plus subcutaneous prime
vaccination with a dual antigen COVID-19
vaccine elicits T-cell and antibody responses in
mice. Scientific Reports, 77(1).
https://doi.oig/10.1038/s41598-021-94364-5
Sadarangani, M., Marchant, A., & Kollmann,
T. R. (2021). Immunological mechanisms of
vaccine-induced protection against COVID-
in humans. Nature Reviews Immunology,
(8). https://doi.org/10.1038/s41577-021-
-z
Sahin, U., Muik, A., Derhovanessian, E., Vogler,
L, Kranz, L. M., Vormehr, M., Baum, A.,
Pascal, K., Quandt, J., Maurus, D.,
Brachtendorf, S., Lorks, V., Sikorski, J., Hilker,
R., Becker, D., Eller, A. K., Griitzner, J.,
Boesler, C., Rosenbaum, C., ... Tiireci, O.
(2020). COVID-19 vaccine BNT162bl elicits
human antibody and TH1 T cell responses.
Nature, 586(7836).
https://doi.oig/10.1038/s41586-020-2814-7
Sauer, K., & Harris, T. (2020). An Effective
COVID-19 Vaccine Needs to Engage T Cells.
Frontiers in Immunology, 11.
https://doi.org/10.3389/fimmu.2020.581807
Sette, A., & Crotty, S. (2021). Adaptive
immunity to SARS-CoV-2 and COVID-19.
In Cell (Vol. 184, Issue 4).
https://doi.Org/10.1016/j.cell.2021.01.007
Smith, C. C,, Olsen, K. S., Gentry, K. M.,
Sambade, M., Beck, W., Garness, J.,
Entwistle, S., Willis, C., Vensko, S., Woods,
A., Fini, M., Carpenter, B., Routh, E.,
Kodysh, J., O’Donnell, T., Haber, C., Heiss,
K., Stadler, V., Garrison, E., ... Rubinsteyn,
A. (2021). Landscape and selection of vaccine
epitopes in SARS-CoV-2. Genome Medicine,
(). https://doi.org/10.1186/sl3073-021-
-1
Tarke, A., Sidney, J., Methot, N., Yu, E. D., Zhang, Y., Dan, J. M., Goodwin, B., Rubiro, P., Sutherland, A., Wang, E., Frazier, A., Ramirez, S. L, Rawlings, S. A., Smith, D. M., da Silva Antunes, R., Peters, B.,Scheuermann, R. H., Weiskopf, D., Crotty, S,, ... Sette, A. (2021). Impact of SARS-CoV-2 variants on the total CD4+ and CD8+ T cell reactivity in infected or vaccinated individuals. Cell Reports Medicine, 2(7). https://doi.org/!0.1016/j.xcrm.2O21.100355
Woldemeskel, B. A., Dykema, A. G., Garliss, C. C„ Cherfils, S., Smith, K. N„ & Blankson, J. N. (2022). CD4+ T cells from COVID-19 mRNA vaccine recipients recognize a conserved epitope present in diverse coronaviruses. Journal of Clinical Investigation, 132(5). https://doi.org/10.1172/JCI156083
Downloads
Published
Issue
Section
License
You are free to:
- Share — copy and redistribute the material in any medium or format for any purpose, even commercially.
- Adapt — remix, transform, and build upon the material for any purpose, even commercially.
- The licensor cannot revoke these freedoms as long as you follow the license terms.
Under the following terms:
- Attribution — You must give appropriate credit , provide a link to the license, and indicate if changes were made . You may do so in any reasonable manner, but not in any way that suggests the licensor endorses you or your use.
- No additional restrictions — You may not apply legal terms or technological measures that legally restrict others from doing anything the license permits.
Notices:
You do not have to comply with the license for elements of the material in the public domain or where your use is permitted by an applicable exception or limitation .
No warranties are given. The license may not give you all of the permissions necessary for your intended use. For example, other rights such as publicity, privacy, or moral rights may limit how you use the material.