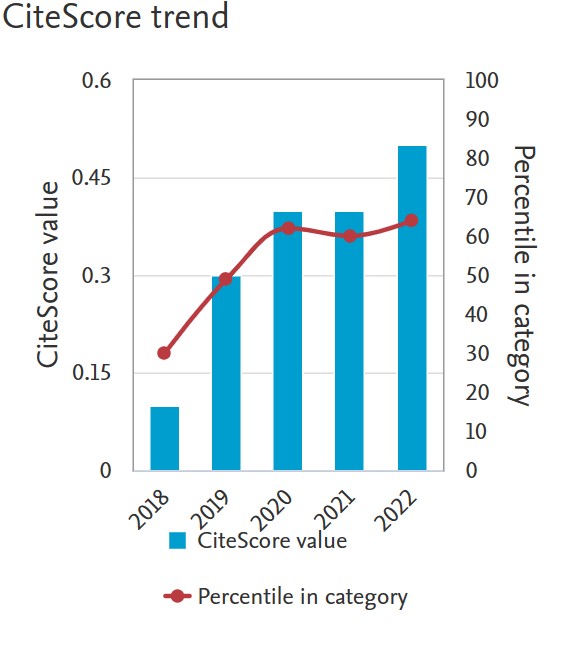
Dynamic effect of zinc on fungal infection in IBD patients
Keywords:
Inflammatory, Candida spp,Aspergillus .pencillium,Mucor.Rhizopus.Saccharomycsis ,Zinc,PCRAbstract
The current study involved 150 samples, 50 for Ctohp’u ravigpvu, 50 for ulcerative colitis patients, and 50 control samples from Al-Kindy teaching hospital in Baghdad. The study aim to investigate the effect of zinc on fungal infection in IBD patients We isolated and named five different yeast species, including C. albicans, C. glabrata, tropicalis C. parapsilosis, C. and C., krusi C. parapsilosis, and Aspergillus, Penicillium, Muocer, Rhizopous, Saccharomycosis, and Cryptococcus. The most common fungus isolated from IBD patients, and the proportions were as follows (andida spp.74%, Aspergillus spp.12%, Penicillium spp. 6%, Mucor spp. 3%, Rhizopus spp. 2%, Saccharomyces spp. 2% and Cryptococcus spp.1%. Likewise, the most common species was Candida albicans isolated from Crohn's patients (Candida albicans 58.54%, Candida glabrata 26.86%, Candida tropicalis 12.2% and Candida krusi 2.44%), with a highly significant difference P. value (<0.001**). The findings of Zinc showed that the mean in CD and UC patients were 45.66±2.86 mg/dL and 48.78±2.59 mg/dL compared to those found in the control group 62.43±2.93 mg/dL with highly significant differences (p≤ 0.0001**). Moreover, Zinc in early and treated IBD patients had the mean values of 48.85±4.97 mg/dL in and 42.21±2.49 mg/dL in CD and 50.61±3.27 mg/dL and 45.79±4.25 mg/dL comparing UC with the control group 62.43±2.93 mg/dL with a highly significant difference (p≤ 0.0001**). Zinc serum level has a strong impact on fungal infections in IBD patients. Also, there was a highly significant difference among all under studied. According to the results,the PCRemployingthe fungi starter pair (ITS1, ITS4) created various molecular sizes (510-870) bp
Downloads
References
Abdul-Hussein, S.S., Ali, E.N., Alkhalidi, N.M., Zaki, N.H. and
Ad'hiah, A.H., 2021. Roles of IL-17A and IL-23 in the Pathogenesis of Ulcerative Colitis and Crohn's Disease.
Iraqi Journal of Science, pp.2526-2535
Ad'hiah, A.H., Jasim, H.A. and Fadhil, A.M.A., 2008. HLA
antigens and inflammatory bowel disease in a sample of
Iraqi patients. EMHJ-Eastern Mediterranean Health
Journal, 74 (5), 1155-1163, 2008.
Ali, A.S., Al-Attraqhchi, A.A. and Al-Ahmar, S.D., 2015.
Molecular detection of ALS1 virulence gene of Candida
albicans isolated from groups of Iraqi patients. Journal
of the Faculty of Medicine Baghdad, 57(1), pp.79-83.
Drshim, A.A., 2005. passive immunization with Candida albicans
antiproteinase as a prophylactic tool against the
candidiasis.Journal of the Faculty of Medicine Baghdad, 47(2),
pp.159-161.
Hamzah, K.J. and Hasso, S.A., 2019. Molecular prevalence of
Anaplasma phagocytophilum in sheep from Iraq. Open
veterinary journal, 9(3), pp.238-245.
Jebur, N.J., Kadhim, D.J. and Firhan, N.M., 2018. Belief about
Medications among Sample of Iraqi Patients with
Inflammatory Bowel Disease. Iraqi Journal of
Pharmaceutical Sciences (P-ISSN 1683-3597 E-ISSN
-3512), pp.32-41.
Mahood,W.S.(2013).Study of some molecular markers alterations in
some Iraqi patients with Colorectal cancer.Ph.D.thesis,Genetic
Engineering and Biotechnology Institute for Postgraduate
studies,Universityof Baghdad:199pp.
Matare, T., Nziramasanga, P., Gwanzura, L., & Robertson, V.
(2017a). Experimental Germ Tube Induction in Candida
albicans: An Evaluation of the Effect of Sodium
Bicarbonate on Morphogenesis and Comparison with
Pooled Human Serum. BioMed Research International,
, 1976273.
McAuliffe, M.E., Lanes, S., Leach, T., Parikh, A., Faich,G., Porter, J.,
Holick, C., Esposito, D., Zhao, Y. and Fox, I., 2015. Occurrence
of adverse events among patients with inflammatory bowel
disease in the HealthCore Integrated Research
Database. Current Medical Research and Opinion, 31(9),
pp.1655-1664.microbiology, 7. 208.
Muhsen, T.A., Hawar, S.N., Mahdi, T.S. and Khaleel, R., 2020.
Effect of Eucalyptus and Myrtus extracts identification
by gas chromatography-mass spectrometry on some
species of Candida as amodel of medical plants. Ann.
Trop. Med. and Public Health, 23(S10), pp.1-11.
Mutar Mahdi, B., 2011. Auto-antibodies in patients with
inflammatory bowel disease unclassified. Iranian Journal
of Immunology, 8(3), pp.189-194.
Sands, B.E. and Ooi, C.J., 2005. A survey of methodological
variation in the Crohn's disease activity
index. Inflammatory bowel diseases, 11(2), pp.133-138.
Trojanowska, D., Zwolioska-Wcis+o, M., Tokarczyk, M.( Kosowski,
K., Mach, T. and Budak, A., 2010. The role of" Candida" in
inflammatory bowel disease: estimation of transmission of"
C. albicans" fungi in gastrointestinal tract based on genetic
affinity between strains. Medical Science Monitor,16(10).
Underhill, D.M. and Braun, J., 2022. Fungal microbiome in
inflammatory bowel disease: a critical assessment. The
Journal of Clinical Investigation, 132(5).
Waly, A.H.T., Barraj, A.H. and Alrikabi, M.H., 2022. Estimation of
Calprotectin, IL-17, and IL-23 levels in the Blood of Iraqi
Patients with Crohn's Disease. The Egyptian Journal of
Hospital Medicine, 88(1), pp.3699-3702.
Zhang, L., Yan, K., Zhang, Y., Huang, R., Bian, J., Zheng, C.,
Sun, H., Chen, Z., Sun, N., An, R. and Min, F., 2007. Highthroughput synergy screening identifies microbial
metabolites as combination agents for the treatment of
fungal infections. Proceedings of the National Academy
of Sciences, 704(11), pp.4606-4611. Mill, J. and Lawrance,
I.C., 2014. Preventing infective complications in
inflammatory bowel disease. World Journal of
Gastroenterology: WJG, 20(29), p.9691.
Li, X.V., Leonardi, I. and lliev, I.D., 2019. Gut mycobiota in
immunity and inflammatory disease. Immunity, 50(6),
pp.1365-1379.
Sokol, H., Leducq, V., Aschard, H., Pham, H.P., Jegou, S.,
Landman, C., Cohen, D., Liguori, G., Bourrier, A., NionLarmurier, I. and Cosnes, J., 2017. Fungal microbiota
dysbiosis in IBD. Gut, 66(6), pp.1039-1048.
Graeser, Y. and Saunte, D.M., 2020. A hundred years of
diagnosing superficial fungal infections: Where do we
come from, where are we now and where would we like
to go?. Acta Dermato-Venereologica,100(9), pp.216-224.
Mullis, K.B. (1990).The unusual origin of the polymerase
chain reaction. Sci. Am., 262(4),56-
Lukdc, N. and Massdnyi, P., 2007. Effects of trace elements
on the immune system. Epidemiologie, mikrobiologie,
imunologie: casopis Spolecnosti pro epidemiologii a
mikrobiologii Ceske lekarske spolecnosti JE Purkyne,
(1), pp.3-9.
Hojyo, S. and Fukada, T., 2016. Roles of zinc signaling in the
immune system. Journal of immunology research, 2016.
Bird, A.J.; Wilson, S. Zinc homeostasis in the secretory pathway
in yeast. Curr. Opin. Chern. Biol. 2020, 55,145-150.
Wilson, D. (2021). The role of zinc in the pathogenicity of
human fungal pathogens. Advances in Applied
Microbiology, 117, 35-61.
Amich, J.; Vicentefranqueira, R.; Mellado, E.; Ruiz-Carmuega,
A.; Leal, F.; Calera, J.A. The ZrfC alkaline zinc transporter
is required for Aspergillus fumigatus virulence and its
growth in the presence of the Zn/Mn-chelating protein
calprotectin. Cell Microbiol. 2014, 16, 548-564.
Fritsch, J., Garces, L., Quintero, M.A., PignacKobinger, J.,
Santander, A.M., Fernandez, I., Ban, Y.J., Kwon, D.,
Phillips, M.C., Knight, K. and Mao, Q., 2021. Low-fat, highfiber diet reduces markers of inflammation and dysbiosis
and improves quality of life in patients with ulcerative
colitis. Clinical gastroenterology and hepatology, 19(6),
pp.1189- 1199
Bradley, I.F., Arce, N.M., Escrig, M.M. and Del Vai, J.H., 2019.
Pulmonary aspergillosis in a Crohn's disease patient
receiving adalimumab and steroid
therapy. Gastroenterologia y hepatologia, 42(6), pp.387-
Leiferman, K.M., Clinical features and diagnosis of bullous
pemphigoid and mucous membrane pemphigoid.
UpToDate [Internet]. 2019;[cited 2019 Aug 01].
Diekema, D.J., Messer, S.A., Hollis, R.J., Jones, R.N. and
Pfaller, M.A., 2003. Activities of caspofungin,
itraconazole, posaconazole, ravuconazole, voriconazole,
and amphotericin B against 448 recent clinical isolates of
filamentous fungi. Journal of Clinical Microbiology, 41(8),
pp.3623-3626.
Chowdhary, A., Kathuria, S., Agarwal, K., Sachdeva, N.,
Singh, P.K., Jain, S. and Meis, J.F., 2014, September.
Voriconazole-resistant Penicillium oxalicum: an
emerging pathogen in immunocompromised hosts.
In Open forum infectious diseases (Vol. 1, No. 2, p.
ofu029). Oxford University Press.
Iwaya, H., Kashiwaya, M., Shinoki, A., Lee, J.S., Hayashi, K., Hara, H.
and Ishizuka, S., 2011. Marginal zinc deficiency exacerbates
experimental colitis induced by dextran sulfate sodium in
rats.TheJournal of Nutrition, 747(6), pp.1077-1082..
Wong, C.P., Rinaldi, N.A. and Ho, E., 2015. Zinc deficiency
enhanced inflammatory response by increasing immune
cell activation and inducing IL6 promoter demethylation.
Molecular nutrition & food research, 59(5), pp.991-999.
Zupo, R., Sila, A., Castellano, F., Bringiotti, R., Curio, M., De
Pergola, G., De Nucci, S., Giannelli, G., Mastronardi, M.
and Sardone, R., 2022. Prevalence of zinc deficiency in
inflammatory bowel disease: a systematic review and
meta-analysis. Nutrients, 74(19), p.4052.
Zhai, X., Wu, H., Wang, Y., Zhang, Z., Shan, L., Zhao, X.,
Wang, R., Liu, C., Weng, Y., Wang, Y. and Liu, X., 2022.
The fruit glossiness locus, dull fruit (D), encodes a C2H2-
type zinc finger transcription factor, CsDULL, in
cucumber (Cucumis sativus L.). Horticulture Research, 9,
p.uhac146.
Citiulo, F., Jacobsen, I.D., Miramon, P., Schild, L., Brunke, S.,
Zipfel, P., Brock, M., Hube, B. and Wilson, D., 2012.
Candida albicans scavenges host zinc via Pra1 during
endothelial invasion. PLoS pathogens, 8(6), p.e1002777.
White, T.J., Bruns, T.D., Lee, S.B. and Taylor, J.W. (1990)
Amplification
and Direct Sequencing of Fungal Ribosomal RNA Genes for
Phylogenetics. In: Innis, M.A., Gelfand, D.H., Sninsky, J.J. and
White,
T.J., Eds., PCR Protocols: A Guide to Methods and
Applications,
Academic Press, New York, 315-322.
Al-Abassi, H.M., Nazal, M.F., Ad'hiah, A.H., Mushe'al, K.I.,
Mubarak, I.H., Alqaisy, I.A., Saadi, A.W. and Kadhim,
S.S., 2015. Serum profile of cytokines in Iraqi
inflammatory bowel disease patients. Mustansiriya
Medical Journal,14(2), pp.11-16.
Downloads
Published
Issue
Section
License
You are free to:
- Share — copy and redistribute the material in any medium or format for any purpose, even commercially.
- Adapt — remix, transform, and build upon the material for any purpose, even commercially.
- The licensor cannot revoke these freedoms as long as you follow the license terms.
Under the following terms:
- Attribution — You must give appropriate credit , provide a link to the license, and indicate if changes were made . You may do so in any reasonable manner, but not in any way that suggests the licensor endorses you or your use.
- No additional restrictions — You may not apply legal terms or technological measures that legally restrict others from doing anything the license permits.
Notices:
You do not have to comply with the license for elements of the material in the public domain or where your use is permitted by an applicable exception or limitation .
No warranties are given. The license may not give you all of the permissions necessary for your intended use. For example, other rights such as publicity, privacy, or moral rights may limit how you use the material.