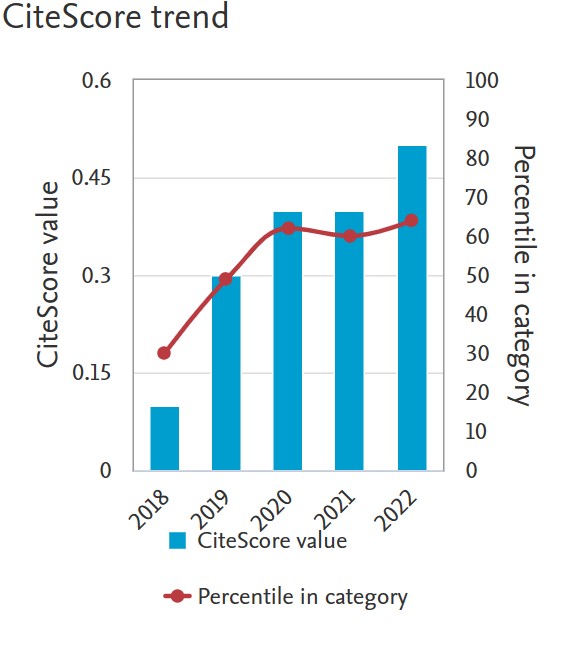
Vitamin D and bone density in chronic hepatitis C patients
Keywords:
Hepatitis, Alkaline phosphatase, BMD, Hepatitis C Virus, Chronic HCV,Abstract
Objective, As bone fragility is common in chronic hepatitis c the study asses to determine the level of vitamin D and bone density and to demonstrate the consequence of vitamin d insufficiency in patient of long standing hepatitis C. Material and Method, 45 individuals were taken as samples, patients with chronic HCV. DEXA was suggested to patients as a follow-up for their condition. An experienced radiology technician has been used as DEXA to evaluate the bone mineral density BMD on the anteroposterior lumbar spine views, bone markers also were evaluated in patient group and control group. Results The study found there was no significant difference between femoral neck and the spine in BMD between HCV patient and control group. The Trochanter and total femur BMD values of HCV mean show significantly low in the experimental group compare to healthy group. Bone mass measurements, Trochanter value (p-value =0.004) and all biochemical parameter are not significantly differed for patients compared to control. Conclusion, The study found no significant difference between viral hepatitis patients and control healthy subjects. Additionally, there was no significant differences in biochemical bone markers for other group
Downloads
References
D. Lavanchy, “Evolving epidemiology of
hepatitis C virus,” Clin. Microbiol. Infect.,
vol. 17, no. 2, pp. 107–115, 2011, doi:
1111/j.1469-0691.2010.03432.x.
M. S. Lin et al., “Association between hepatitis C
virus infection and osteoporotic fracture risk
among postmenopausal women: A crosssectional investigation in Taiwan,” BMJ
Open, vol. 9, no. 1, 2019, doi:
1136/bmjopen-2018-021990.
C. Mazzaro et al., “A review on extrahepatic
manifestations of chronic hepatitis c virus
infection and the impact of direct-acting
antiviral therapy,” Viruses, vol. 13, no. 11, pp.
–20, 2021, doi: 10.3390/v13112249.
[R. A. L. Sutton, S. Mumm, S. P. Coburn, K.
L. Ericson, and M. P. Whyte, “‘Atypical
femoral fractures’ during bisphosphonate
exposure in adult hypophosphatasia,” J.
Bone Miner. Res., vol. 27, no. 5, pp. 987–
, 2012, doi: 10.1002/jbmr.1565.
L. G. S. Orsini, M. M. Pinheiro, C. H. M.
Castro, A. E. B. Silva, and V. L. Szejnfeld,
“Bone mineral density measurements,
bone markers and serum vitamin D
concentrations in men with chronic noncirrhotic untreated hepatitis C,” PLoS
One, vol. 8, no. 11, pp. 8–12, 2013, doi:
1371/journal.pone.0081652.
M. P. Whyte et al., “Rapid skeletal turnover
in a radiographic mimic of osteopetrosis,”
J. Bone Miner. Res., vol. 29, no. 12, pp.
–2609, 2014, doi: 10.1002/jbmr.2289.
J. D. Perkins, “Techniques to ensure adequate
portal flow in the presence of splenorenal
shunts,” Liver Transplant., vol. 13, no. 5,
pp. 767–768, 2007, doi: 10.1002/lt.
P. Thakur et al., “Proximal Hip Geometry,
Trabecular Bone Score, Bone Mineral
Density and Bone Mineral Parameters in
Patients With Cryptogenic and Hepatitis B
Related Cirrhosis- A Study From the
Indian Subcontinent,” J. Clin. Densitom.,
vol. 25, no. 1, pp. 97–104, 2022, doi:
1016/j.jocd.2021.03.001.
J. T. Mehsen, Z. S. Madhi, and I. S. Madhi,
“Spinal Stenosis : What Outcome Should be
Expected ? Review the Latest Evidence
Using the Assessment of Multiple Systematic
Reviews Appraisal Tool ( AMSTAR ),” pp.
–121, 2020, doi: 10.4103/MJBL.MJBL.
H. Zhao, C. Zheng, M. Zhang, and S. Chen,
“The relationship between vitamin D
status and islet function in patients with
type 2 diabetes mellitus,” BMC Endocr.
Disord., vol. 21, no. 1, pp. 1–7, 2021, doi:
1186/s12902-021-00862-y.
H. K. Bhattarai, S. Shrestha, K. Rokka, and R.
Shakya, “Vitamin D, Calcium, Parathyroid
Hormone, and Sex Steroids in Bone Health
and Effects of Aging,” J. Osteoporos., vol.
, 2020, doi: 10.1155/2020/9324505.
N. M. M. Mansibang, M. G. Y. Yu, C. A.
Jimeno, and F. L. Lantion-Ang,
“Association of sunlight exposure with 25-
hydroxyvitamin D levels among working
urban adult Filipinos,” Osteoporos.
Sarcopenia, vol. 6, no. 3, pp. 133–138,
, doi: 10.1016/j.afos.2020.08.006.
M. Zou et al., “Molecular Analysis of
CYP27B1 Mutations in Vitamin DDependent Rickets Type 1A: c.590G > A
(p.G197D) Missense Mutation Causes a
RNA Splicing Error,” Front. Genet., vol.
, no. November, pp. 1–7, 2020, doi:
3389/fgene.2020.607517.
N. Charoenngam, A. Shirvani, and M. F. Holick,
“Vitamin D for skeletal and non-skeletal
health: What we should know,” J. Clin.
Orthop. Trauma, vol. 10, no. 6, pp. 1082–1093, 2019, doi: 10.1016/j.jcot.2019.07.004.
C. C. Wu et al., “Antiproteinuria Effect of
Calcitriol in Patients With Chronic Kidney
Disease and Vitamin D Deficiency: A
Randomized Controlled Study,” J. Ren.
Nutr., vol. 30, no. 3, pp. 200–207, 2020, doi:
1053/j.jrn.2019.09.001.
H. Pott-Junior, C. Luzeiro, J. F. Senise, and
A. Castelo, “Association of seasonality and
serum albumin concentration with
Vitamin D deficiency in subjects with
chronic hepatitis C infection living in a
sunny country,” Public Health Nutr., vol.
, no. 7, pp. 1247–1253, 2020, doi:
1017/S1368980019004178.
M. B. Humble, S. Gustafsson, and S. Bejerot,
“Low serum levels of 25-hydroxyvitamin
D (25-OHD) among psychiatric outpatients in Sweden: Relations with season,
age, ethnic origin and psychiatric
diagnosis,” J. Steroid Biochem. Mol.
Biol., vol. 121, no. 1–2, pp. 467–470,
, doi: 10.1016/j.jsbmb.2010.03.013.
J. F. Huang et al., “Sustained virological
response to interferon reduces cirrhosis in
chronic hepatitis C: A 1386-patient study
from Taiwan,” Aliment. Pharmacol.
Ther., vol. 25, no. 9, pp. 1029–1037, 2007,
doi: 10.1111/j.1365-2036.2007.03297.x.
S. K. Tohra et al., “Prediction of sustained
virological response to combination
therapy with pegylated interferon alfa and
ribavirin in patients with genotype 3
chronic hepatitis C,” Dig. Dis. Sci., vol.
, no. 8, pp. 2449–2455, 2011, doi:
1007/s10620-011-1770-3.
M. L. Yu et al., “A sustained virological response
to interferon or interferon/ribavirin reduces
hepatocellular carcinoma and improves
survival in chronic hepatitis C: A nationwide,
multicentre study in Taiwan,” Antivir. Ther.,
vol. 11, no. 8, pp. 985–994, 2006, doi:
1177/135965350601100811.
S. A. Gabr and A. H. Alghadir, “Handgrip
Strength and Vitamin D as Predictors of Liver
Fibrosis and Malnutrition in Chronic
Hepatitis C Patients,” Dis. Markers, vol.
, 2021, doi: 10.1155/2021/6665893.
L. N. Hammad, S. M. Abdelraouf, F. S.
Hassanein, W. A. Mohamed, and M. F.
Schaalan, “Circulating IL-6, IL-17 and
vitamin D in hepatocellular carcinoma:
Potential biomarkers for a more favorable
prognosis?,” J. Immunotoxicol., vol. 10,
no. 4, pp. 380–386, 2013, doi:
3109/1547691X.2012.758198.
M. Pinzani, K. Rombouts, and S. Colagrande,
“Fibrosis in chronic liver diseases:
Diagnosis and management,” J. Hepatol.,
vol. 42, no. SUPPL. 1, pp. 22–36, 2005,
doi: 10.1016/j.jhep.2004.12.008.
M. Zheng and R. Gao, “Vitamin D: A
Potential Star for Treating Chronic
Pancreatitis,” Front. Pharmacol., vol. 13,
no. June, pp. 1–15, 2022, doi:
3389/fphar.2022.902639.
“Neonatal cholestasis : new insights into
pathophysiology and strategies to improve
patients ’ diagnosis and prognosis,” 2022.
I. Milosevic et al., “Gut-liver axis, gut
microbiota, and its modulation in the
management of liver diseases: A review of
the literature,” Int. J. Mol. Sci., vol. 20,
no. 2, pp. 1–16, 2019, doi:
3390/ijms20020395.
N. Berlanda, E. Somigliana, P. Viganò, and P.
Vercellini, “Safety of medical treatments
for endometriosis,” Expert Opin. Drug
Saf., vol. 15, no. 1, pp. 21–30, 2016, doi:
1517/14740338.2016.1121991.
M. T. Kitson and S. K. Roberts, “D-livering
the message: The importance of vitamin D
status in chronic liver disease,” J.
Hepatol., vol. 57, no. 4, pp. 897–909,
, doi: 10.1016/j.jhep.2012.04.033.
D. El-Maouche et al., “Controlled HIV viral
replication, not liver disease severity
associated with low bone mineral density
in HIV/HCV co-infection,” J. Hepatol.,
vol. 55, no. 4, pp. 770–776, 2011, doi:
1016/j.jhep.2011.01.035.
C. N. Jin, J. D. Chen, and J. F. Sheng,
“Vitamin D deficiency in Hepatitis C virus
infection: What is old? what is new?,” Eur.
J. Gastroenterol. Hepatol., vol. 30, no. 7,
pp. 741–746, 2018, doi:
1097/MEG.0000000000001134.
Downloads
Published
Issue
Section
License
You are free to:
- Share — copy and redistribute the material in any medium or format for any purpose, even commercially.
- Adapt — remix, transform, and build upon the material for any purpose, even commercially.
- The licensor cannot revoke these freedoms as long as you follow the license terms.
Under the following terms:
- Attribution — You must give appropriate credit , provide a link to the license, and indicate if changes were made . You may do so in any reasonable manner, but not in any way that suggests the licensor endorses you or your use.
- No additional restrictions — You may not apply legal terms or technological measures that legally restrict others from doing anything the license permits.
Notices:
You do not have to comply with the license for elements of the material in the public domain or where your use is permitted by an applicable exception or limitation .
No warranties are given. The license may not give you all of the permissions necessary for your intended use. For example, other rights such as publicity, privacy, or moral rights may limit how you use the material.